In this article
Spironolactone is a long-used prescription medicine that was originally developed as a diuretic. Today, it is also widely used for hormone-related symptoms such as some types of female-pattern hair loss, acne, and unwanted facial hair.
If you are dealing with Hashimoto’s, hypothyroidism, perimenopause/menopause, hair loss, skin changes, or weight concerns, spironolactone sits in an important but often misunderstood space: it can help certain symptoms related to excess male hormones (androgens).
Historically, medical fields have been viewed separately. Thyroid specialists monitor your thyroid, while dermatologists treat hair loss and acne. However, your thyroid hormone status and menopausal changes dictate how your cells respond to androgens. And, if you’re on GLP-1 medications, the mobilization of hormones stored in your fat cells can trigger androgenic flares. Recognizing that your skin and hair are connected to your thyroid and hormonal health will allow you to stop viewing symptoms in isolation and start managing your endocrine system as a whole.
This article looks at the most common questions you may have and what you need to know about spironolactone treatment.
Spironolactone is a diuretic drug with a second life. Its primary use is as a “water pill,” helping the body get rid of excess salt and water while holding onto potassium. That basic kidney-supporting action is why it has been used for blood pressure, heart failure, and fluid retention. Its anti-androgen effects, however, make it interesting for women’s hormonal health and dermatology.
In plain language, spironolactone can reduce the effect of androgens such as testosterone on your skin and hair follicles, which is why clinicians sometimes use it for female-pattern hair loss, hormonal acne, and excess body hair (hirsutism).
People often hear about spironolactone when they are frustrated by symptoms that seem “hormonal” but are hard to fix with diet, supplements, or generic skin care. That includes acne that flares around cycles or midlife, chin hair that suddenly gets coarser, scalp hair thinning, and skin that feels oilier or less predictable than before.
It is also commonly discussed in thyroid communities because thyroid disease and hormonal imbalance often coexist, and hair loss in particular may have more than one cause at the same time.
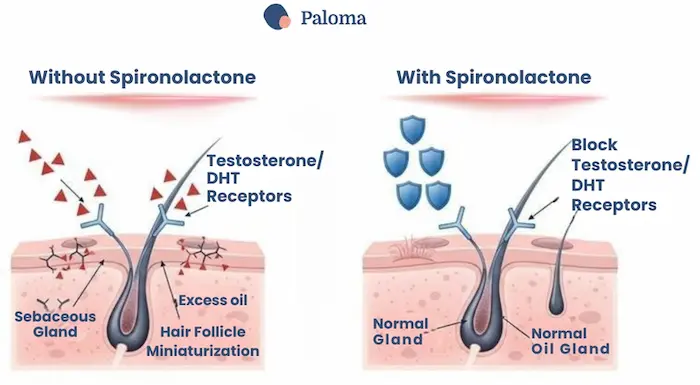
The power of spironolactone lies in its identity as an androgen receptor antagonist. It works by blocking the ability of androgens—like testosterone and dihydrotestosterone (DHT)—to bind to receptors in the oil glands of the skin and the hair follicles. By effectively “turning down the volume” on these androgenic signals, it has two key effects:
- Helps treat acne by reducing oil (sebum) production
- Helps reduce hair loss by preventing the miniaturization of hair follicles.
Thyroid hormones modulate the production and binding of sex hormone-binding globulin (SHBG). When thyroid function is suboptimal, SHBG levels often plummet, leaving more “free” androgens circulating in the bloodstream. This creates a state of excess androgens – known as hyperandrogenism – even if your absolute androgen levels appear within a “normal” range. This is why individuals with Hashimoto’s or hypothyroidism – a deficiency in thyroid hormone –often report thinning hair or sudden, persistent cystic acne that does not respond to standard skin regimens.
It’s important to note that spironolactone is not a treatment for Hashimoto’s thyroiditis or hypothyroidism. Rather, it may help if androgens are contributing to hair loss.
If hair thinning, fatigue, dry skin, constipation, or weight gain are being driven by hypothyroidism, your first priority is usually to make sure thyroid hormone replacement treatment is optimized.
Many patients find that even after optimizing thyroid function, hair and skin concerns persist. This is where the “residual symptom” gap exists. If your thyroid medication has restored energy but your hair and skin are still symptomatic, your receptors may still be hypersensitive to androgens. Spironolactone acts as a secondary shield, protecting your tissues from the effects of those circulating hormones that remain elevated due to the thyroid-mediated SHBG shift. In that situation, your healthcare provider may consider spironolactone as one part of a broader plan, especially if your hair loss looks more like female-pattern hair loss than diffuse “thyroid shedding.”
A practical way to think about it is this: thyroid treatment supports the whole system, while spironolactone may help if androgens are acting like an extra brake on hair follicles or skin.
Midlife can bring a frustrating hormonal shift. As estrogen falls, the relative effect of androgens may become more noticeable. This drop in estrogen can show up as acne along the jawline, new facial hair, or scalp thinning. Spironolactone is commonly used in this setting because it targets androgen-driven changes rather than directly targeting estrogen levels.
For some women, it can be particularly appealing if they are not candidates for estrogen therapy, do not want it, or are already using hormone therapy but still have skin or hair symptoms. It is important, though, that spironolactone is not a menopause “fix-all”; it addresses specific symptoms, not the menopausal transition itself.

Hair loss is a multifaceted problem. Telogen effluvium is a reactive hair shedding caused by systemic stress, such as rapid weight loss, surgery, nutritional deficiencies, or thyroid fluctuation. Androgenic alopecia, conversely, is hair thinning driven by excess DHT.
Distinguishing between the two is vital.
Spironolactone is specifically effective for female-pattern hormonal hair loss, as it stops the progression of androgen-sensitive follicle miniaturization. Research suggests that some women experience reduced shedding, improved thickness, or regrowth over time, though responses vary, and benefits usually take months rather than weeks.
That timing matters. Hair cycles are slow, so people sometimes quit too early because they expected quick results. Spironolactone is generally a slower treatment for hair loss than a rapid reset.
When the body is under metabolic stress, hair follicles are often the first to be sacrificed. By blocking androgen receptors, Spironolactone provides a “protective buffer” for the hair follicles. It keeps the environment around the follicle stable, preventing the hormonal surges associated with metabolic adjustment from worsening the underlying hair thinning.
Hair loss can also be an adverse effect of GLP-1 medications used for weight management. GLP-1 medications significantly reduce appetite and, by extension, nutrient intake. Hair health is highly dependent on protein, iron, and zinc status. If you are not absorbing enough nutrients due to altered gastric emptying, your hair will suffer regardless of your hormonal profile. Spironolactone works best when combined with an optimized nutritional strategy, ensuring you aren’t just protecting the follicles from hormones but also fueling them with the raw materials they need.
Spironolactone has become a familiar option for hormonal acne, especially jawline or lower-face breakouts that seem stubborn and cycle-linked. It is also used for hirsutism, meaning unwanted coarse hair growth on the face or body.
These effects happen because the drug reduces the impact of androgen signaling, which can lower oil production and calm the hormone-driven cascade behind acne and hair growth. Many people notice acne improvement first, while hair and facial-hair changes usually take longer.
Spironolactone is not a weight-loss medication. Because it is a diuretic, some people may temporarily see a drop on the scale from fluid loss, but that is not the same as losing body fat.
This distinction matters a lot for people with hypothyroidism, perimenopausal weight gain, or medication-related weight changes. If the concern is weight management, body composition, appetite, metabolism, or insulin resistance, spironolactone is not designed to solve those problems. It may occasionally help with “puffiness” or fluid retention, but it should not be viewed as a weight loss drug.
Spironolactone may be most helpful for people who have a pattern of:
- Hormonal acne, especially on the jawline or chin area.
- Unwanted facial or body hair.
- Female-pattern hair loss.
- Midlife androgen-related skin or hair changes.
Spironolactone is less likely to help if the main issue is untreated hypothyroidism, low iron, scalp inflammation, or another non-androgen cause of hair loss. That is why a good workup is important.
Most people tolerate spironolactone reasonably well, but common side effects include increased urination, dizziness, breast tenderness, fatigue, and menstrual irregularities. The most important serious risk is high potassium (hyperkalemia), especially in people with kidney disease, those taking potassium supplements, or those prescribed certain blood pressure drugs for cardiovascular diseases.
The FDA labeling advises checking potassium within about a week of starting or changing the dose, and then monitoring regularly afterward, with closer follow-up in higher-risk patients. Because the kidneys clear the drug, reduced kidney function raises the risk of complications.
Spironolactone is also not safe in pregnancy because of its anti-androgen effects, so pregnancy avoidance is essential if there is any chance of conception. That is especially relevant for perimenopausal users who may ovulate unpredictably.
For acne, improvement may begin in about 8 to 12 weeks; for hair shedding, changes may take 3 to 6 months or longer. Facial hair changes can also take months, because existing hairs must grow out before you can judge the difference in coarseness.
Because it works gradually, spironolactone is usually best thought of as a maintenance medication rather than a quick rescue. Many patients do best when paired with a broader plan that may include thyroid optimization, iron assessment, scalp-directed treatments such as minoxidil or Propecia, and realistic expectations.
There are some important guidelines to keep in mind when taking spironolactone.
Track your symptoms
When you take multiple medications, careful tracking of symptoms is essential. For example, if you’re taking a GLP-1 drug, nausea and vomiting can be side effects. Still, if they persist alongside dizziness, it may signal an electrolyte imbalance or a drop in blood pressure caused by the addition of spironolactone. You should work with your healthcare provider to isolate these variables, using a log to track symptom onset relative to dose changes.
To log symptoms, create a simple tracking system. Monitor your skin’s oiliness and breakout frequency, the thickness of your ponytail or scalp coverage, and your daily energy. These three metrics provide a clear “scorecard” of your endocrine health. If energy dips while skin improves, you may need to adjust your electrolyte intake. If skin worsens, you may need a dose adjustment.
Monitor electrolytes when combining spironolactone and GLP-1s
Both spironolactone and certain GLP-1 medications affect kidney function and fluid balance. Spironolactone is potassium-sparing, meaning it can raise potassium levels. While this is rarely an issue for healthy individuals, when combined with medications that, like GLP-1s, affect gastric motility or kidney clearance, it necessitates regular monitoring. Work with your doctor to establish a schedule for routine metabolic panels.
Stay well-hydrated
The diuretic effect of spironolactone, combined with the appetite-suppressing, thirst-altering nature of GLP-1s, can easily lead to chronic, low-level dehydration. This dehydration is often the root cause of the nausea and dizziness patients report. Be sure to prioritize electrolyte-rich hydration—not just plain water—to help lessen these common side effects.
Monitor blood pressure and heart rate
Spironolactone naturally lowers your blood pressure. If you are also on other blood pressure or weight loss medications, you must monitor for lightheadedness. Your “target” for heart rate and blood pressure may shift as you lose weight, and your medication dosages should be reviewed at every follow-up visit to ensure you are not over-medicated.
Be patient
Hormonal regulation is a slow process. Improvements to hair and skin usually follow months of consistent spironolactone treatment, not weeks.

At Paloma, we know hormonal skin and hair changes rarely happen in isolation. For many people, spironolactone can be a helpful tool for some types of hair loss, acne, and unwanted facial hair — especially during perimenopause and menopause — but it is only one part of a bigger picture. It does not treat Hashimoto’s or hypothyroidism itself.
Working with Paloma means you get more than a prescription. You get a thoughtful, personalized approach that looks at thyroid health, metabolic treatment, use of GLP-1 medications, hydration, convenient lab testing, and symptom patterns together, so your care plan feels coordinated instead of fragmented. We help you track what is changing, understand what to monitor, and stay patient through the process, because hormonal improvements usually take months, not weeks.
If you are navigating thyroid disease, GLP-1 therapy, or perimenopause/menopause, our team helps you move forward safely with medical supervision and clear guidance. At Paloma, we believe you should feel informed, supported, and actively involved in your own hormonal health journey.
- Spironolactone is a diuretic with anti-androgen effects, commonly used for hair loss, acne, and unwanted hair growth.
- It works by blocking androgen receptors, reducing oil production, and protecting hair follicles from thinning.
- Spironolactone does not treat underlying conditions like hypothyroidism or menopause—only certain symptoms.
- Thyroid dysfunction can increase free androgens, making symptoms like acne and hair loss worse.
- It is most effective for female-pattern hair loss and hormonal acne.
- Results take time—8–12 weeks for acne, and 3–6+ months for hair changes.
- Spironolactone is not a weight-loss drug or helpful in weight management—any scale changes are typically due to temporary fluid loss. It can, however, help address hair loss associated with GLP-1 medications.
- Regular monitoring is important due to side effects like high potassium, especially when combined with other medications.

.webp)

%20copy%202.webp)



%20(1).webp)





